Today, and in the past, women make up the majority of this team including apothecaries’ assistants, nurses, health visitors, midwives, and pharmacists, practice managers, and receptionists.
As GPs moved into group practices from the 1960s, the need and potential for a wider team became increasingly obvious, although appropriate training and pay remained key issues. “Ancillary staff”, as they were known, were encouraged so that doctors could concentrate on their areas of expertise and delegate other secretarial, nursing and book-keeping work.
Originally developed in the USA in the 1960s, the slow start to establish the role of practice managers in the UK allowed for significant increase in expertise.
General practice is considered unique for its relatively flat professional hierarchy, with an increasingly complex workload shared across multidisciplinary teams. These relationships are a key element in the wider conversation around personalised care and continuity, especially when considering patients with multiple needs.
“We must pass on everything that can be done as well, or better, by ancillaries than we do it ourselves.” Man GP, 1962
“Steering a course between the needs and wishes of the patient and the availability and capabilities of the doctor.” Survey result, 1974
“The district nurse is of course a firm friend and ally. Man GP, 1960s
“The challenge for the future appears to be how to develop an expanded clinical role for nurses in general practice while minimising role conflict and overlap with doctors.” Ann Bowling, 1981
Key dates
1948 Introduction of the National Health Service
1964 Association of Medical Secretaries established
People
Find out more about individual women’s experiences by clicking to expand.

Helen Kilminster is Senior Pharmacist at the Tower hill Partnership Medical Practice, Primary Care Network (PCN) Clinical Director for the People’s Health Partnership, PCN Clinical Director Board Member, West Midlands NHS Confederation, and Vice President of the Primary Care Pharmacy Association.
“General practice was never an obvious career choice for me. However, I was presented with an opportunity seven years ago to demonstrate what pharmacists could do for general practice teams and how my skill set could benefit patients in primary care. As a working mum, general practice allows me to create some flexibility in my diary and I do attempt to balance work commitments with home life and professional commitments. I fully recognise my own limitations but also the biases I encounter as a woman of BAME background and as a pharmacist. General practice has given me challenges that have tested my mindset and my ability to persist professionally and as an individual. The relationships and trust I have built with team members since working in general practice have given me courage and autonomy to push myself to be a better clinician.
The increasing number of visible female leaders in general practice is encouraging but I feel there is still further progress to be made. The new power of authentic leadership may often be wrongly perceived as weak and emotional, but I hope that my approach enables our Primary Care Network to continue to evoke positive changes and career opportunities for future pharmacy professionals.”

Kari Millar trained as a registered general nurse, working in varied nursing roles to fit around her family commitments, before moving to Westburn Medical Group in Aberdeen, initially as a nurse, but since 2010 as practice manager.
“Having become disillusioned with hospital nursing, in September 1988 I applied for a part-time practice nurse post at Westburn Medical Group. I felt valued and was able to combine working with family life.
“I have seen general practice change over the years. Increased autonomy of nurses, encouraged to deliver increased roles, becoming the lead for chronic disease management, promoting health.
“I became involved in the College’s Quality Practice Award scheme which the practice gained in 1996, then became an assessor for practice visits. Audit and quality are so important for good patient care and I felt very supported in following my goal.
“General practice management followed in 2010 and I have kept my nurse registration up to date. I feel the move from hospital to general practice allowed the best progression for me in a professional sense while allowing good quality family life. I appreciate the opportunities general practice has given me to promote patient care through my management of the practice.”
Stories
Waiting room display
The introduction of practice nurses was linked to changes to GPs’ reimbursements and expenditure allowances in the 1960s which made it more economically sensible to employ ancillary staff, as well as move surgeries to group practices and out of the family home. Numerous reports in the 1960s and 1970s concluded that GPs found that practice nurses eased their workload, raised clinical and technical standards, and could extend the scope of the practice.
Between 1977 and 1987, this system was used at Hanover House Practice, Tonbridge, to call patients in the downstairs waiting room by pressing a button on each GP’s desk. Although the partners changed during this period, there was always a practice nurse. Credit: Sharon Messenger.
Practice nurse weekly schedule, 1970
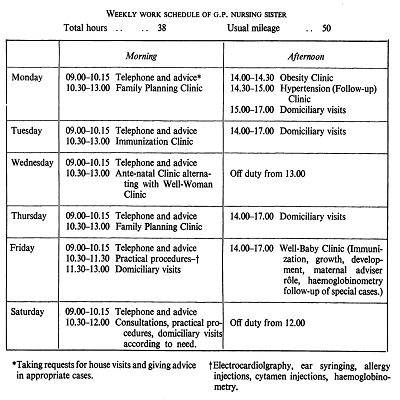
The early 1960s marked a time of transition from district nurses to practice nurses. From their introduction, practice nurses typically carried out vaccinations, injections, dressings, treating ear and eye complaints, and running family planning, and baby and infant clinics. These services were supported by district nurses, midwives and health visitors, all also primarily women.
GP nursing sister schedule, 1970. Credit: BJGP.
Gemma Barnett performs her award-winning spoken word poem The Front Desk, which draws on the experience of being a GP’s receptionist during the COVID pandemic.
Voices
Listen as Ann Telesz describes changes to the roles of practice manager and practice nurse, John Ford discusses the process of repeat prescription before computers with Sharon Messenger, and Robert MacGibbon recalls his conception of the receptionist role.
Transcripts

Discover the exhibition
Find out more about the history of women in general practice by visiting our Women in GP exhibition.
Thank you for your feedback. Your response will help improve this page.
